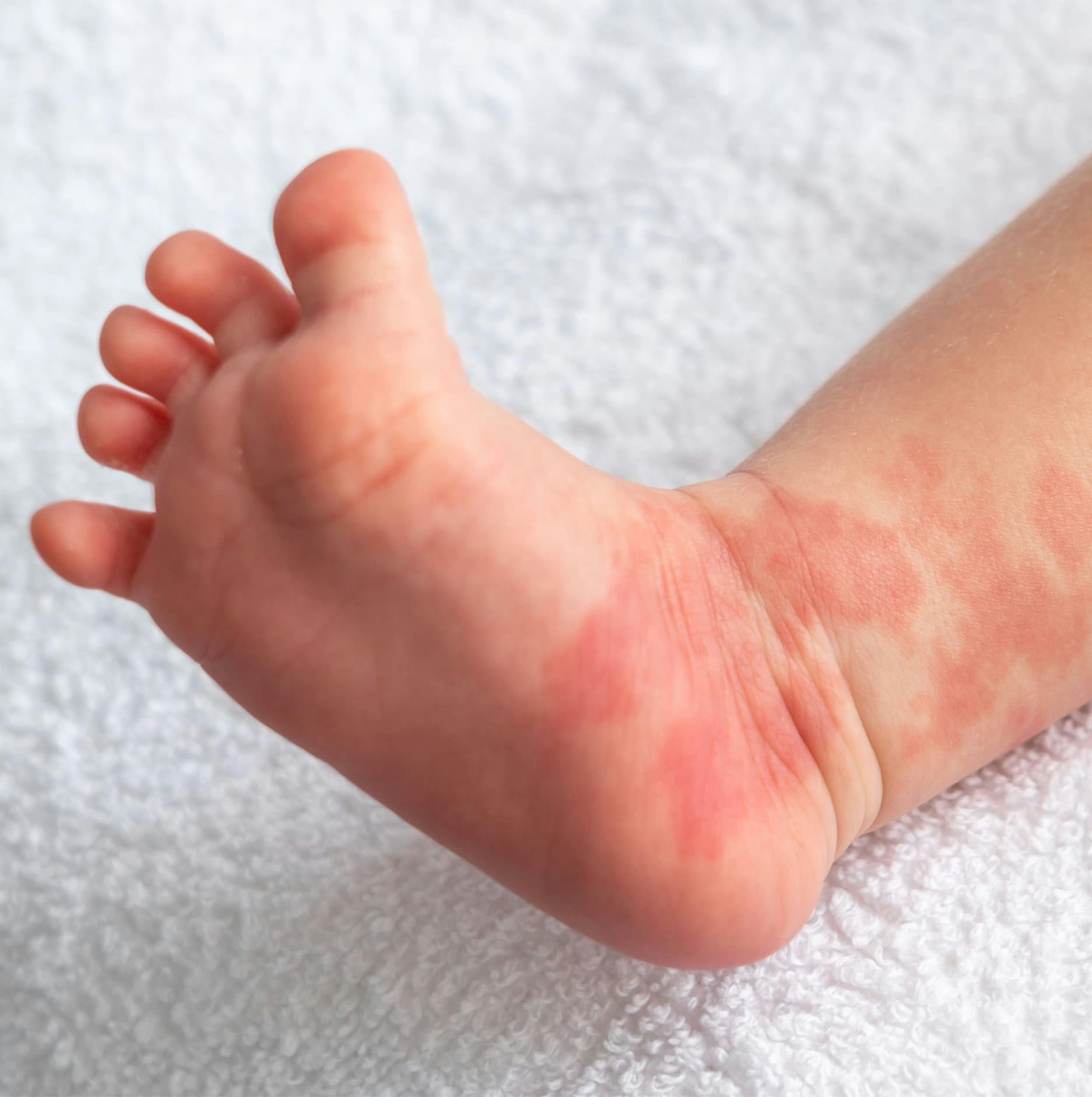
This is the most common type of vascular birthmark, affecting roughly 1 in 10 children. Most hemangiomas are of the infantile type and tend to go through a well-described cycle of growth followed by involution. The treatment of hemangiomas can range from simple observation to surgical excision.
Types of Hemangiomas
Hemangiomas come in two main varieties: infantile and congenital.
Infantile Hemangiomas
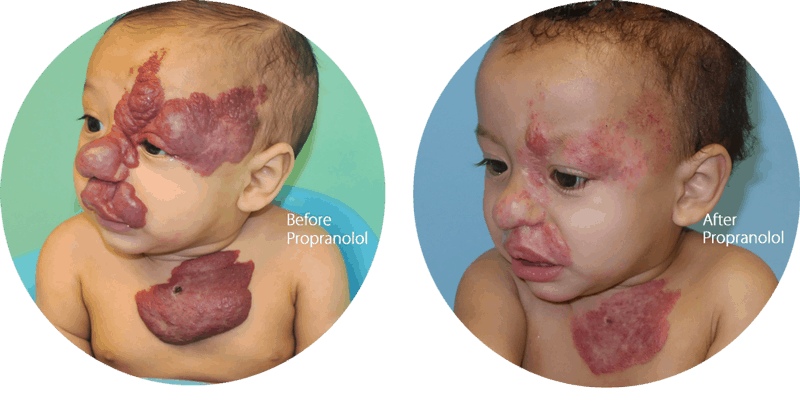
These types of hemangiomas are usually not present at birth, and they start growing after birth. They look red and grow rapidly. Subtypes of infantile hemangiomas are:
- Superficial Hemangiomas, or “strawberry” hemangiomas, appear as bright red tumors.
- Deep Hemangiomas can appear under or on the skin that may appear normal or have a bluish hue.
- Mixed Hemangiomas have both superficial and deep components.
- Nodular hemangioma is the most common form. They are discreet and oval or round. Besides, these hemangiomas tend not to have a connection with malformations.
- Large hemangiomas with characteristic geographic shapes that span a wide area of the body can be a sign of greater complications and underlying developmental issues.
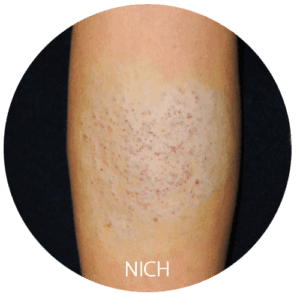
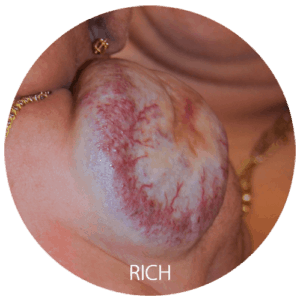
Congenital Hemangiomas
Prenatal ultrasounds can detect hemangiomas, which are vascular lesions that have developed in the uterus and are present at birth. These lesions usually appear round or oval and may be pink, purple, or a mixture of colors. Additionally, the skin growth is usually raised and warm to the touch.